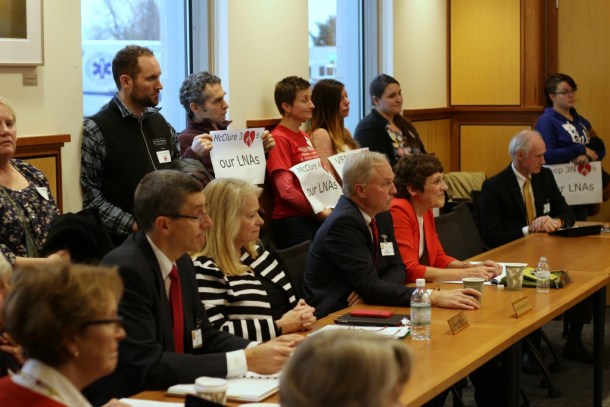
[B]URLINGTON — Hundreds of support workers at the University of Vermont Medical Center say they’re being overworked, underpaid, and need a labor union to protect them.
The group of licensed nursing assistants and mental health technicians have been filling out union cards saying they want to join the Vermont Federation of Nurses and Health Professionals. That union already represents registered nurses who work in the hospital.
Under state law, if the group of LNAs, mental health technicians and related workers can get enough cards filled out, they can elect a collective bargaining representative.
However, because the LNAs and mental health technicians are legally considered part of a larger bargaining unit that includes other hospital support staff, they are asking the hospital to allow just the LNAs and mental health technicians to bargain collectively.

To that end, dozens of LNAs attended the hospital’s board of trustees meeting on Thursday afternoon to tell the administration why they should be allowed to join the union. The group also brought allies, including members of Rights and Democracy and the Vermont Workers Center.
“The work of nurse’s aides and the work of frontline health care providers is so crucial,” said James Haslam, the executive director of Rights and Democracy. “I’ve been here (as a patient) on nights when there hasn’t been enough staff, and you’re wondering and you’re looking for answers.”
LNAs take a course after graduating from high school and get licensed through the state to take care of patient needs like bathing and changing bedpans. Mental health technicians, who have CPR and de-escalation training, sit with psychiatric patients, especially when patients are potentially suicidal. The LNAs say they’re often asked to fill in for mental health technicians.
The workers are seeking to have the hospital hire more LNAs and mental health technicians to reduce their workloads, to pay a base wage of $15 per hour, to pay incentives when they are called in at the last minute, and to set a maximum number of patients they should be responsible for every shift.
Sheena Maynard, an LNA, said the starting wage for an LNA is between $11 and $12 per hour, but the hospital is so understaffed that sometimes an LNA will be called in at the last minute to serve 20 or 30 patients at a time.
“The staffing crisis that we have experienced puts patients in difficult and sometimes dangerous situations and needs to be addressed immediately,” Maynard told the board.
She said when LNAs see call lights indicating that a patient needs help, they are supposed to respond within two minutes. Recently, she said those lights have been left on for up to 15 minutes.
“People are laying in their stool and their urine because we don’t have time to get there,” said Daniel Doynow, another LNA. “We don’t feel … like we’re really being respected.”
Doynow added: “We’re just looking for better working conditions. We want to be able to offer the best care possible. It’s hard to leave and see a coworker crying because she or he wasn’t able to take care of a patient.”
After the event, the hospital released the following statement: “We recognize the right of the LNA group to organize. We’ll work with them through the process governed by federal law.”
